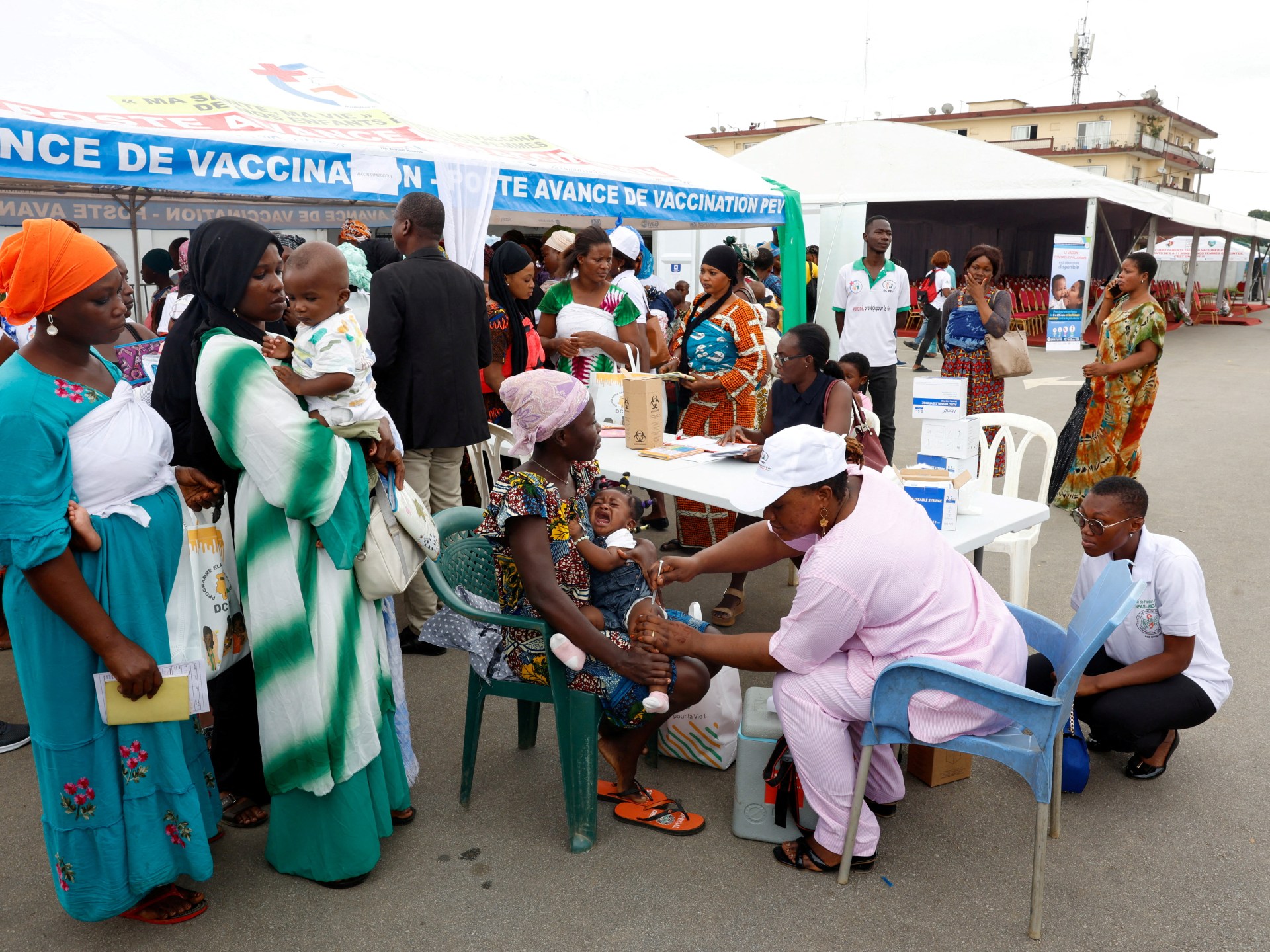
Mosquitoes are commonly associated with serious diseases, such as malaria, dengue fever and yellow fever, however, researchers from Leiden University Medical Center and Radboud University in the Netherlands may have found these insects have a valuable new role, as vaccine providers.
Scientists at these universities say they have successfully engineered mosquitoes to deliver vaccines that could provide significantly enhanced immunity against malaria.
The latest global report on malaria issued by the World Health Organization revealed that an estimated 597,000 people died from malaria overall in 2023, most of them in African countries, which account for 95% of malaria deaths.
Scientists estimated that more than 240 million cases of malaria occur annually around the world, noting that children and pregnant mothers are most vulnerable to contracting the disease.
How does the mosquito vaccine work?
The vaccine uses a weakened strain of the parasite that causes the most dangerous form of malaria in humans (Plasmodium falciporum). “We removed an important gene in the malaria parasite, and this allows it to infect people without making them sick.”
The malaria parasite is usually transmitted to humans through the bite of a mosquito, which uses its proboscis to penetrate the skin, and injects its saliva into the bloodstream before absorbing the blood. The parasites in the saliva are transmitted directly to the liver, where they multiply rapidly, before leaving the liver and infecting red blood cells with malaria. This leads to malaria. Symptoms such as fever, chills, and sweating.
In the clinical trial, the research team used mosquitoes carrying the modified parasite to deliver the vaccine via bites. This reflects the natural transmission of malaria, and the goal is to create a strong immune response in the liver and thus protect against malaria infection.
“Because the gene is turned off, this parasite cannot complete its development in the liver, cannot enter the bloodstream, and therefore cannot cause symptoms of the disease,” Rostenberg said. “At least that was the theory.”
How were the experiments conducted?
The first trial tested an injectable malaria vaccine derived from a genetically modified parasite known as PfSPZ GA1. The study, in collaboration with Sanara, a US-based biotechnology company that develops vaccines, included 67 participants from two cities in the Netherlands (Leiden and Nijmegen).
The results of the study, published in May 2020 in the journal Science Translational Medicine, showed that the GA1 vaccine was safe to use, and it delayed the onset of malaria but did not prevent the participants from developing malaria. from contracting the disease.
In the second trial, participants, none of whom had previously suffered from malaria, received two versions of the mosquito-borne vaccines GA1 and a modified version of GA2.
In the GA1 vaccine, the parasite multiplied in the liver over a 24-hour period. In the GA2 vaccine, the parasite multiplied over a longer period of time, up to a week, and this allowed the immune system more time to recognize it and begin fighting it.
The researchers first tested doses of the “GA2” vaccine on the participants to determine its safety and tolerability. Then the participants were divided into 3 groups. Two groups tested the “GA1” and “GA2” vaccines, respectively, and the first group was given a placebo.
In each of the three sessions, participants received 50 mosquito bites, 8 from GA1-infected mosquitoes, nine from GA2-infected mosquitoes, and 3 from uninfected mosquitoes. Participants who completed the vaccination phase then received 5 Bites from mosquitoes carrying the malaria parasite.
What are the results?
The results of the study were published in November in the New England Journal of Medicine. According to it, 13% of the group infected with GA1 and 89% of the group infected with GA2 developed immunity to malaria, and no one in the group developed Placebo immunity to malaria.
Is more research needed?
Experts said that the GA2 vaccine still needs to be tested in larger studies because the sample size in the clinical trial was small (20 participants).
More research is also needed to determine how successful the GA2 vaccine is in boosting the immune system over longer periods of time, and whether it can protect against different strains of the malaria parasite in areas where the disease is widespread.
“Using mosquitoes as a vector is the easiest and fastest way to deliver malaria spores,” Rostenberg explained. She added: “Of course, this is not sustainable in the long term, and therefore the product will have to be developed as a vaccine packaged in a vial to be launched in Africa.”
She added, “Mosquitoes cannot be used to deliver vaccines on a large scale. This is only possible in the context of a clinical trial.”
Have insects been used to deliver vaccines before?
Japan 2010
In 2010, Japanese scientists genetically modified mosquitoes to carry a vaccine against leishmaniasis, a parasitic disease spread in the salivary glands usually by sand flies. The vaccine is expressed in the mosquito’s saliva as it bites.
The study showed that rodents bitten by the “flying vaccines” developed antibodies to the parasite. However, researchers have not yet determined whether the resulting immune response was sufficient to prevent infection.
“After bites, protective immune responses are stimulated, just like traditional vaccination, but without the pain and without the cost,” lead researcher Shigeto Yoshida of Jichi Medical University said in a statement.
United States 2022
In September 2022, a study including 26 participants in Seattle, Washington, explored the potential of mosquitoes as pollinators.
In an experiment similar to the one conducted in the Netherlands, mosquitoes served as carriers of malaria-causing Plasmodium parasites that had been genetically weakened using gene editing technology. This was the first significant clinical trial to use mosquitoes as a direct vaccine delivery system with genetically modified parasites.
Participants were first given the malaria vaccine and then given the malaria virus to see if the vaccine would protect them from infection.
The mosquito-delivered vaccine was 50% effective, with 7 out of 14 participants contracting the disease.